Hashimoto’s encephalopathy (HE) impacts the brain and how it functions. Hashimoto’s encephalopathy symptoms include seizures, disorientation, altered behavior, and cognitive difficulties.
There have also been reports of psychosis, which includes visual hallucinations and paranoid delusions. HE primarily affects adults and more frequently affects females than males.
Although the precise origin of HE is unknown, an aberrant immunological or inflammatory response may be involved. Hashimoto’s thyroiditis and HE are linked; however, it’s unknown how they are connected.
The symptoms, clinical examination, and laboratory tests diagnose HE. It might be necessary to rule out more frequent conditions initially.
Table of Contents
ToggleWhat Is Hashimoto’s Encephalopathy?
Rare ailment Hashimoto’s encephalopathy (HE) is most likely autoimmune. “Autoimmunity” refers to diseases where the immune system unintentionally targets the body’s cells.
Although Hashimoto’s brain degeneration can affect people of any age, it most frequently affects women over 50. We also know from recent research on other types of autoimmune encephalitis that HE may not be a single diagnosis but a syndrome that combines several distinct illnesses.
As a result, many different Hashimoto’s encephalopathy symptoms and indicators exist.
What Are the Hashimoto’s Encephalopathy Symptoms?
Hashimoto’s encephalopathy impacts your brain’s physiological processes, leading to cognitive deterioration and altered consciousness. Typically, one of these three things happens:
1. Relapsing & Remitting
Acute symptom episodes frequently involve seizures and attacks resembling strokes come and go.
2. Progressive
Cognitive Hashimoto’s brain degeneration develops over time into dementia, hallucinations, disorientation, disturbances of the sleep-wake cycle, or even a coma.
3. Self-limiting
The sickness goes away independently after a symptomatic period and without medical intervention.
Hashimoto’s encephalopathy symptoms include:
- Depression, which may be the first symptom of the progressive form
- Fatigue
- Anxiousness
- Over-responsive reflexes
- Poor appetite
- Confusion
- Cerebral ischemia (lack of blood flow to areas of the brain)
- Altered consciousness
- Tremors
- Disorientation
- Concentration and memory problems
- Psychosis and delusional behavior
- Spasms and jerks in the muscles known as myoclonus
- Lack of muscle coordination, which can cause difficulty walking
- Speech problems
- Headaches
- Lack of concentration and inattentiveness
- Emotional instability
- Withdrawal from social activities
- Personality changes
What Are the Causes of Hashimoto’s Brain Degeneration?
Although the specific etiology of Hashimoto’s brain degeneration is unknown, researchers believe that, like Hashimoto’s thyroiditis, HE is an autoimmune disorder in which the body’s immune system erroneously attacks its tissues for pathogens or viruses.
The brain is the intended target in the case of HE. In Hashimoto’s thyroiditis, the thyroid gland is attacked by the immune system, which results in hormonal issues. The connection between these ailments is still a mystery.
What Is the Diagnosis of Hashimoto’s Encephalopathy?
There is currently no conclusive test for Hashimoto’s encephalopathy available to medical professionals. HE is simple to misdiagnose or ignore because your brain is the primary target of its symptoms. Sometimes, Creutzfeldt-Jakob disease, dementia, Alzheimer’s disease, or stroke are misdiagnosed in patients.
First, other recognized causes of encephalopathy must be ruled out. Next, thyroid dysfunction and the presence of certain antibodies—the immune system’s “attack” cells—must be checked for.
Causes of Encephalopathy
The term “encephalopathy” is used by medical research as a general term for illnesses that affect the structure or function of the brain but lacks a clear definition.
Numerous illnesses cause this, including chronic, acute (short-term), and irreversible diseases. Chronic encephalopathies are typically brought on by the brain experiencing long-term changes. They consist of the following:
- Traumatic brain injury
- Heavy metal exposure
- HIV-related changes
- Korsakoff encephalopathy
- Spongiform encephalopathies such as Creutzfeldt-Jakob
Acute encephalopathies include transient functional abnormalities brought on by:
- Toxins
- Metabolic disturbances
- Combinations of the above causes
Blood tests may be performed depending on the factors your doctor thinks are most plausible.
- Antithyroid Antibodies
Testing for thyroid peroxidase (TPO) and antithyroglobulin (TG) antibodies, two thyroid-attacking antibodies, is essential since they are required to diagnose HE due to their elevated levels in the body.
- Thyroid Hormone Levels
Thyroid hormone levels are typically assessed due to their different levels in each individual. According to research, patients may show the following levels of Thyroid-stimulating hormone:
- Subclinical hypothyroidism (low hormone levels below the cutoff for thyroid illness).
- Primary hypothyroidism (underactive thyroid disease)
- Hyperthyroidism (overactive thyroid disease)
Studies have also revealed that patients with Hashimoto’s encephalopathy may have normal levels of TSH, and the majority may have no signs of previous thyroid disease.
- Ruling Out Other Causes
Testing for and excluding other potential causes of your symptoms is a key component of HE diagnosis.
1. Lumbar Puncture
A lumbar puncture, sometimes referred to as a spinal tap, checks your cerebrospinal fluid for elevated protein levels, which are found in around 75% of HE cases. The fluid can also be cultured to identify any bacteria, viruses, or other pathogens that might cause the symptoms.
2. Electroencephalography (EEG)
Your brainwaves are measured using electrodes during a non-invasive examination called electroencephalography (EEG). 90% to 98% of persons with Hashimoto’s encephalopathy have abnormalities.
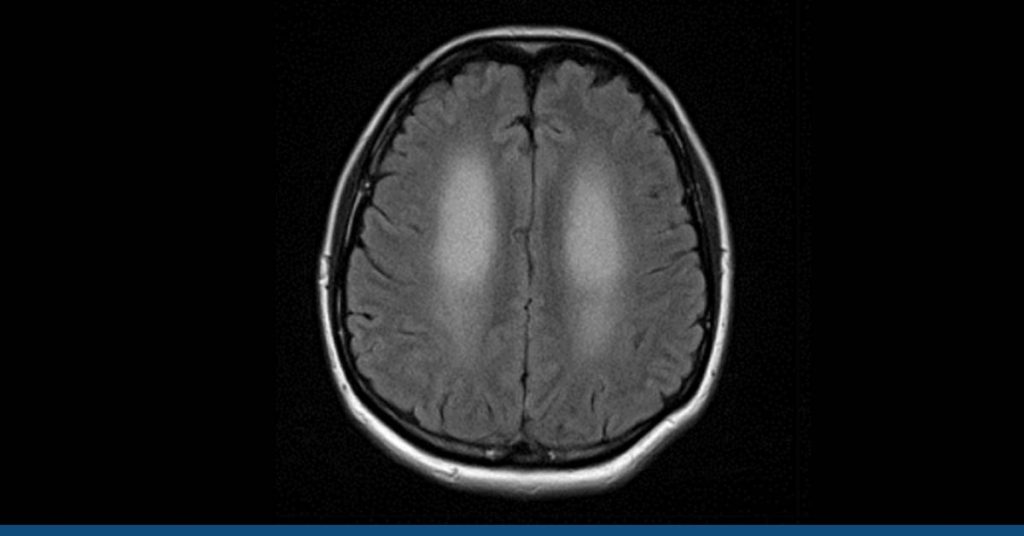
3. Magnetic Resonance Imaging (MRI)
Detailed brain images are produced via magnetic resonance imaging (MRI).
What Is the Treatment of Hashimoto’s Brain Degeneration?
Oral corticosteroids, mostly prednisone, or intravenous (IV) Medrol, are the main treatments for Hashimoto’s encephalopathy (methylprednisolone).
Most patients respond successfully and fast to medication therapy, with symptoms of improvement or the condition going away within a few months.
One characteristic that distinguishes Hashimoto’s encephalopathy is the response to steroid therapy. The following solutions are available for those who cannot take corticosteroids or whose symptoms did not improve after taking them:
1. Immunosuppressive Medication
Immunosuppressive drugs such as Rituxan, Cytoxan, or CellCept (mycophenolate mofetil) (rituximab) are prescribed.
2. Intravenous Immunoglobulin
Intravenous immunoglobulin (IVIG) delivers antibodies from healthy donors to the patient. It aids in the removal of unwanted antibodies and inhibits their activity.
3. Plasma Exchange
In plasma exchange, dangerous antibodies are removed by extracting the patient’s plasma (the liquid in your blood) and replacing it with healthy plasma.
Conclusion
Hashimoto’s encephalopathy causes brain degeneration. Its symptoms include memory loss, confusion, and seizures. Although the exact etiology is uncertain, Hashimoto’s thyroiditis is suggested to be a possible relation.
HE is difficult to diagnose, and it requires excluding other potential causes, looking for particular antibodies, and keeping track of thyroid function.
Fortunately, even if they aren’t diagnosed for a while, most patients benefit from therapy with steroids or other medicines.
The HG Analytics provides screening and diagnostic options that allow us to detect Hashimoto’s encephalopathy using MRI and EEG.
Our medical specialists with extensive knowledge and experience handle consultations.
You will receive a thorough report detailing your results and any recommendations for additional testing or treatment that may be required. So, book your consultation now.