Heart failure results when the heart cannot pump enough blood to meet the body’s needs. Decompensated heart failure (DHF) is the stage in which the symptoms become so severe that they require immediate medical attention.
The symptoms, such as shortness of breath, fatigue, and fluid retention, worsen.
DHF may be new (acute), or the result of worsening symptoms from previously occurred heart failure (an aggravation).
It is a deadly diagnosis, with mortality and morbidity rates frequently exceeding those of viral and malignant diseases.
Since decompensated heart failure is a complex illness, it is frequently treated with multiple methods concurrently.
Read on to find everything about decompensated heart failure, including symptoms, prevention, and treatment options.
Table of Contents
ToggleWhat Is Decompensated Heart Failure (DHF)
Decompensated heart failure is characterized by the heart’s inability to pump enough oxygenated blood to meet the body’s metabolic demands.
It is a clinical syndrome that occurs when any anomaly in the structure or function of the heart renders it unable to expel and maintain appropriate blood pressure.
This reduces the heart’s efficiency and necessitates rapid therapeutic intervention. It is referred to as cardiogenic shock. It is a type of heart failure that develops unexpectedly and demands hospitalization and unplanned emergency room visits.
There are two main types of DHF:
Acute DHF
The most common type of heart failure occurs in people without previous failure symptoms. People who previously experienced a heart attack, mitral valve prolapse (structural change), or hypertensive crisis (high BP) are more prone to suffer acute DHF. It may cause pulmonary congestion.
Chronic DHF
It affects people who are already diagnosed with heart failure. The symptoms may develop gradually, or sometimes they present suddenly, requiring immediate medical assistance.
DHF Causes and Symptoms
Acute decompensated heart failure causes include volume overload, pressure overload, and acute contractility dysfunction.
Fluid therapy can increase preload, resulting in heart failure symptoms such as shortness of breath, low oxygen levels, pulmonary congestion, peripheral edema, mental state abnormalities, and end-organ dysfunction. Increased preload impairs the myocardium’s ability to contract, making it difficult for the left ventricle (LV) to raise stroke volume.
As the pain induces sympathetic stress responses, the blood capillaries constrict, increasing the afterload. The LV cannot overcome the high resistance when myocardial contractility is low.
This causes a decrease in stroke volume and acute heart failure symptoms. Myocardial infarction (MI) and issues with the functioning of the heart’s valves can both contribute to the start of contractility failure.
The common causes of chronic DHF are pulmonary embolism, bradyarrhythmia, infection, and the use of anti-inflammatory drugs.
Decompensated congestive heart failure is also related to hypervolemia. Heart failure affects normal renal (kidney) functioning, impacting the kidney’s ability to excrete sodium from the body. As a result, there is water retention leading to fluid overload.
The common symptoms of decompensated congestive heart failure include:
- Shortness of breath
- Peripheral edema
- Pulmonary congestion
- Hypoxemia
- Elevated jugular venous pressure
- Pleural effusion
DHF Diagnosis and Treatment
The symptoms, biochemical data, and imaging examinations of a patient can help physicians diagnose decompensated heart failure.
Due to reduced blood flow, the patient’s physical examination indicators include pulmonary auscultation, jugular venous distention, and cold extremities.
Biochemical Data
Biomarkers B-type natriuretic peptide (BNP) and N-terminal fragment pro-BNP (NT-proBNP) can detect heart failure. BNP readings greater than 500 pg/mL and NT-proBNP values greater than 300 pg/mL have a 90% likelihood of being accurate.
A full metabolic profile can be useful when evaluating liver and renal issues brought on by enlarged veins and poor blood flow. In addition, laboratory data can be utilized to determine the source of electrolyte disorders such as hyponatremia and hypokalemia.
Imaging Techniques
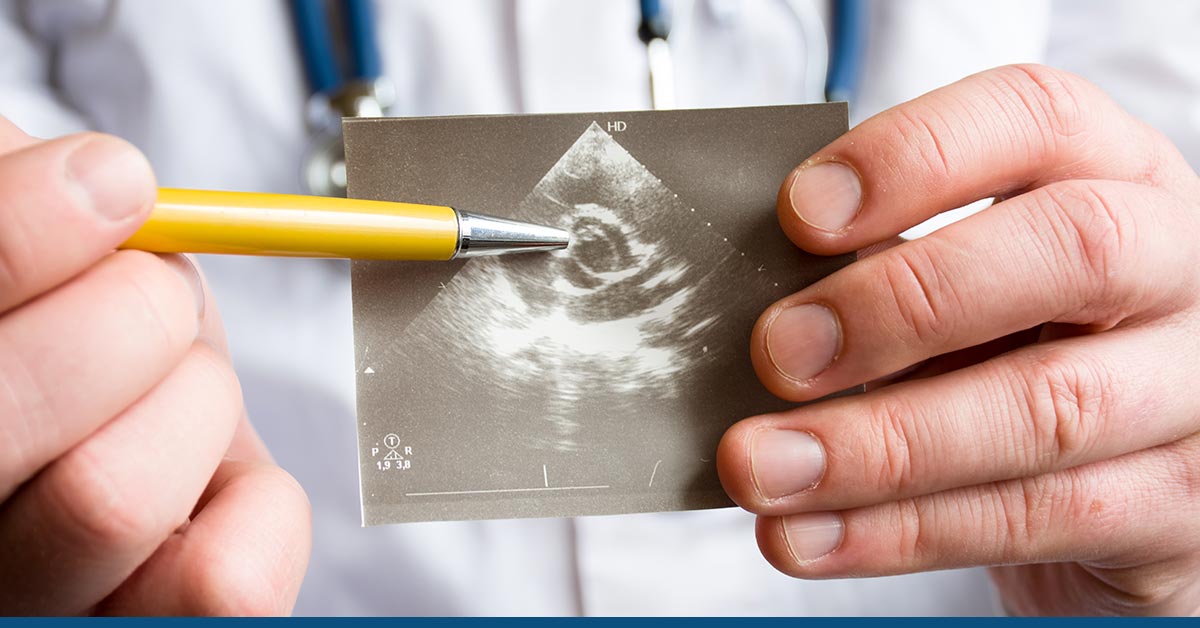
Transthoracic echocardiography is a sophisticated imaging technique that provides visual and numerical data in real-time on the size, thickness, systolic and diastolic function, and presence or absence of structural anomalies in the heart’s chambers. This information may be obtained by placing a transducer on the patient’s chest. It can be used to diagnose the patient and determine how to treat them.
A chest x-ray may reveal pulmonary vein congestion, interstitial emphysema, or an enlarged heart. Typically, the findings of a radiographic exam are available up to 12 hours after the onset of the first symptoms of an illness.
Treatment Options
Patients with acute heart failure are treated by addressing the condition’s underlying cause. To increase the contractility of the heart muscle, loop diuretics, which reduce preload and diastolic ventricular wall stress, can be employed. Exhibiting diuretics, patients with indicators of volume excess often find relief from their symptoms.
This is accomplished by eliminating congestion in the pulmonary and peripheral systems as early as possible.
Medications that reduce afterload make it simpler for persons with heart failure caused by pressure overload to beat their hearts. Both stroke volume and cardiac output will increase when the smooth muscles of the blood arteries relax.
Inodilators could be administered to patients with worsening symptoms who have not responded to the prescribed medication.
These medications can cause the heart muscle to contract more forcefully and reduce the resistance of the blood arteries throughout the body. Consequently, cardiac output and systemic perfusion are enhanced.
When treating acute heart failure, it is vital to avoid medications that reduce the activity of the heart muscle, such as beta-blockers.
If a patient continues to have symptoms such as altered mental status, chilly and clammy extremities, rising lactate levels, and deteriorating end-organ dysfunction, the medical treatment for decompensated heart failure may be deemed unsuccessful.
Needle devices could be utilized in this instance to assist the heart temporarily. They assist the LV during cardiogenic shock, a severe heart failure condition. VA-ECMO is a novel technique since it can support both ventricles simultaneously.
The life expectancy of a person with decompensated heart failure varies on factors such as age, gender, and the presence or absence of other chronic conditions. People with DHF have a greater chance of living a long and good life if they receive effective treatment.
DHF Prevention
It is crucial to consume a healthy diet to prevent heart failure. Reduce your consumption of sugar, salt, and saturated and trans fats.
You should instead concentrate on consuming fruits and vegetables, low-fat dairy products and proteins, and lean meats. Olive oil, walnuts, avocados, salmon, and tuna are all excellent sources of healthy, i.e., unsaturated fats.
Conclusion
Decompensated heart failure is characterized by breathing difficulties, edema, and pulmonary effusion. Valve disease, high blood pressure, or an irregular heartbeat increase the likelihood of experiencing heart failure.
Medical specialists might recommend the optimal treatment for heart failure based on the severity of a patient’s condition. Screening should be utilized to determine a person’s risk for heart failure or heart disease.
A simple, painless, and noninvasive test can determine your risk. HG Analytics’ preventive wellness program offers a painless screening to detect the earliest signs of many conditions impacting the heart.
Consult us if you are concerned about your health in any manner, and we will assist you in determining what is wrong and what to do about it. Book your consultation now.
More On Heart-Related Issues:
- Is Belching a Sign of Heart Attack?
- What is Compensated Heart Failure? Everything you need to know
- Stroke Vs. Heart Attack: Difference You Should Know
- What is the Life Expectancy with Leaky Heart Valve?
- Heart Palpitations and Headache – Causes and Symptoms
- Fluid Around Heart – Causes, Symptoms, and Treatment
- Should An Irregular Heartbeat Worry Me?
- Does Your Heart Stop When You Sneeze?
- What Distinguishes A Heart Attack From Heart Failure?